

Understanding the procedure, success rates, recovery, and life after a heart transplant. Essential facts and figures for patients and families.

Dr. Michael Chen
Cardiac Surgeon & Transplant Specialist
A heart transplant is a surgical procedure performed on patients with end-stage heart failure or severe coronary artery disease when other medical or surgical treatments have failed. Since the first successful human-to-human heart transplant performed by Dr. Christiaan Barnard in 1967, this life-saving procedure has evolved dramatically, with survival rates improving significantly due to advancements in surgical techniques, organ preservation, and immunosuppressive medications.
Today, approximately 3,500 heart transplants are performed worldwide each year, with the United States accounting for about half of these procedures. Despite these numbers, the demand far exceeds the supply of available donor hearts, creating a critical need for more organ donors and advancements in artificial heart technology.
Heart transplantation is considered for patients with end-stage heart failure when all other treatment options have been exhausted. Common conditions leading to transplant evaluation include:
To be considered for transplant, patients must meet specific criteria:
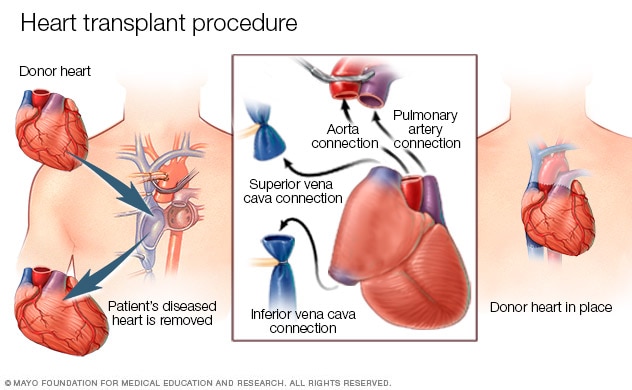
A heart transplant is a complex procedure typically lasting 4-8 hours. The surgery involves removing the diseased heart and replacing it with a healthy donor heart. Here's what happens:
The donor heart is carefully removed from the deceased donor and preserved in a cold solution. The maximum ischemic time (time without blood flow) is typically 4-6 hours.
The recipient is placed on cardiopulmonary bypass, which takes over the function of the heart and lungs during surgery.
The surgeon removes most of the recipient's diseased heart, leaving portions of the atria to which the donor heart will be attached.
The donor heart is connected to the recipient's blood vessels and remaining atrial tissue. The surgical connection points are called anastomoses.
The new heart is warmed and restarted. The patient is gradually weaned from cardiopulmonary bypass as the transplanted heart takes over circulation.

Survival rates for heart transplant recipients have improved significantly over the past decades due to better surgical techniques, improved immunosuppressive medications, and enhanced post-transplant care.
| Time Period | Survival Rate | Key Factors Influencing Survival |
|---|---|---|
| 30 Days | 95% | Surgical complications, donor heart quality, recipient condition |
| 1 Year | 91% | Acute rejection, infection, primary graft dysfunction |
| 5 Years | 75-80% | Chronic rejection, cardiac allograft vasculopathy, renal dysfunction |
| 10 Years | 55-60% | Long-term complications of immunosuppression, malignancies, chronic rejection |
| 20 Years | 20-25% | Late graft failure, age-related comorbidities, long-term medication effects |
Recovery from a heart transplant is a gradual process that requires close medical supervision and significant lifestyle adjustments. The average hospital stay is 10-14 days, followed by several months of intensive outpatient monitoring.
Despite significant advancements, heart transplantation still faces several challenges and potential complications that require careful management.
The immune system recognizes the transplanted heart as foreign and attacks it. Acute rejection occurs in 30-40% of patients within the first year.
A unique form of coronary artery disease that develops in the transplanted heart, affecting up to 50% of recipients by 10 years post-transplant.
Immunosuppressive medications increase susceptibility to infections, particularly in the first year post-transplant.
Long-term immunosuppression increases cancer risk, particularly skin cancers and lymphoproliferative disorders (10-15% at 10 years).
Immunosuppressants can cause kidney damage, hypertension, diabetes, osteoporosis, and neurological side effects.
Heart transplantation remains the gold standard treatment for end-stage heart failure, offering significantly improved survival and quality of life compared to medical therapy alone. With current 1-year survival rates exceeding 90% and median survival approaching 15 years, it represents one of modern medicine's most remarkable achievements.
However, significant challenges remain, particularly the critical shortage of donor organs. Only about 25-30% of patients on waiting lists receive a transplant each year. Future directions in heart transplantation include:
As research continues and technology advances, heart transplantation will continue to evolve, offering hope to the thousands of patients worldwide suffering from end-stage heart failure.

Cardiac Surgeon & Transplant Specialist
Dr. Chen has performed over 300 heart transplant procedures and leads the cardiac transplant program at Gods Life Health Care. He has 15+ years of experience in advanced heart failure management.
Get the latest cardiac health insights and transplant advancements delivered to your inbox.